Publications
- Join the BSP
- Awards
- Awards & Prizes 2020
- Awards & Prizes 2021
- Awards & Prizes 2022
- Awards & Prizes 2023
- Awards & Prizes 2024
- Awards & Prizes 2025
- Awards & Prizes 2026
- Implant Information for GDPs
- BSP Webinars - 2018 Classification System
- BSP UK Version of the S3 Treatment Guidelines for Periodontitis
- Clinical FAQs - practitioner top tips and helpful videos
- Healthy Gums Do Matter toolkit
- Infographics
- Perio and Caries
- Periodontal Disease and Diabetes
- Job Vacancies
- EFP Manifesto
- EFP Prevention Workshop Guidelines
BSP Commercial Use and Distribution Policy
One of the aims of the BSP is to promote the art and science of periodontology and dental implantology. To achieve this aim, we allow many of our resources to be downloaded and printed for your personal use, non-commercial teaching, research purpose or private study.
We will not allow any of our documentation to be amended, nor will we allow it to be hosted on any other websites or social media platforms. We are the owners of the copyright in many of the documents and any breach of these terms will be considered an infringement of our rights under the Copyright, Designs and Patents Act 1988. Furthermore, a breach of this policy may result in legal action.
If you wish to reproduce a BSP resource in a publication then please seek permission in writing from the Executive General Manager, Paula Dunn (admin@bsperio.org.uk). Such requests will be presented to BSP Council and their decision will be final. Any permissions granted will require an acknowledgement to be included in the publication giving credit for the resource to the BSP.
Patient Leaflet - Periodontal health for a better life
BSP Clinical Guidelines
Clinical Information
Delivering better oral health: an evidence-based toolkit for prevention

Public Health England published the fourth edition of "Delivering Better Oral Health: an evidence based toolkit for prevention" on the 21st September 2021. The publication can be found here: https://www.gov.uk/government/publications/delivering-better-oral-health-an-evidence-based-toolkit-for-prevention
This updated toolkit will help both dental teams and wider health and social care professionals alike to provide high quality preventative care and advice to their patients and people in their care. It can also be used as an evidence-based teaching resource. We wish to highlight the key new elements:
- Delivering Better Oral Health: an evidence based toolkit for prevention (fourth edition) has been developed through a wider UK collaboration of experts, frontline practitioners and for the first time patient representatives
- The toolkit has been published on gov.uk in a new digital format making it easily accessible on mobile devices
- Although the summary tables (chapter 2) have not changed significantly, there is new content on:
- infant feeding
- early detection of oral cancer and more detail on tobacco cessation and alcohol reduction
- a new table on tooth wear focusing on accelerated tooth wear
In addition, the importance of effectively supporting behaviour change is acknowledged with this chapter, coming immediately after the summary guidance tables, with practical examples as case studies. Throughout the new version of DBOH there has been a greater consideration of the oral health of older people and other vulnerable groups.
A holistic approach to patient care
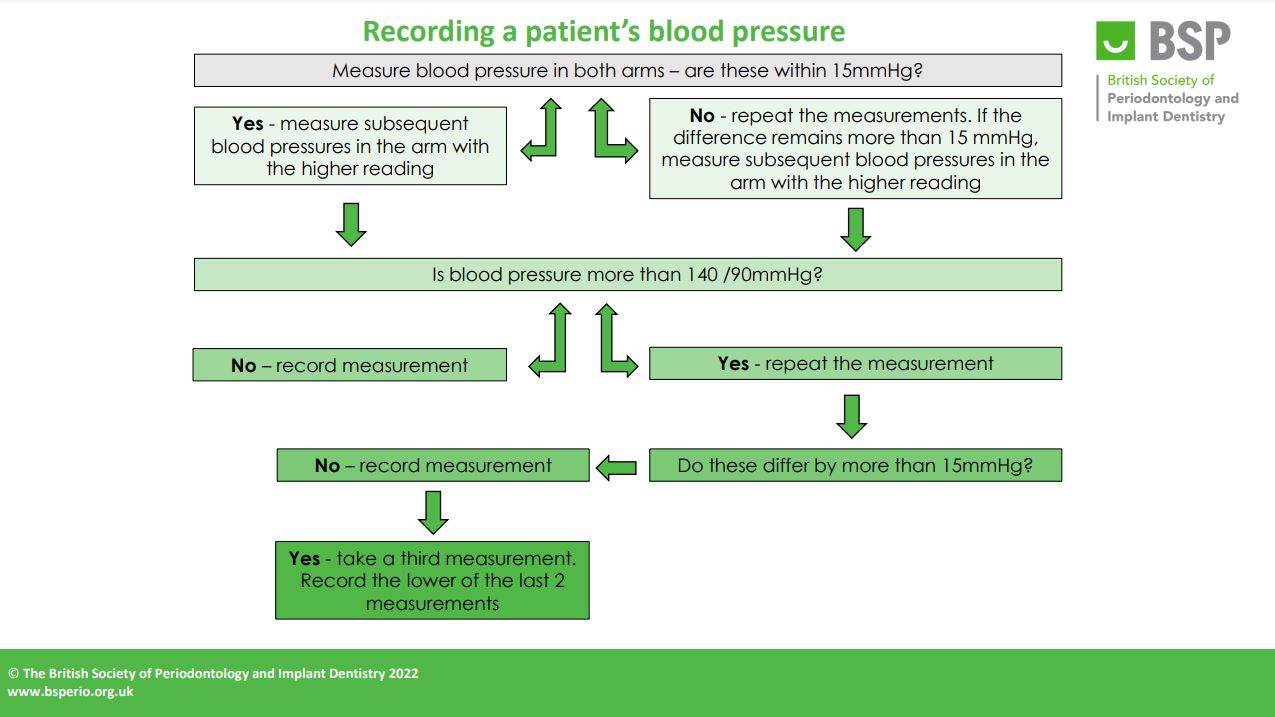
Some dental care professionals choose to screen their patients when attending for a periodontal assessment and routinely record height, weight and waist measurements together with blood pressure. Having calculated their patient’s body mass index (BMI), they may discuss lifestyle factors, such as smoking, alcohol, diet and exercise.
Research has shown that increased body mass index (BMI) and waist measurements are associated with several common chronic diseases, including high blood pressure, heart disease and type 2 diabetes.
Diabetes and smoking are the major risk factors for periodontitis. Whilst this is not yet formally acknowledged in treatment guidelines, there is a growing body of scientific data suggesting that higher BMI is associated with the extent and severity of periodontitis and potentially also treatment outcomes. This is in addition to our belief that periodontitis may be a modifiable risk factor for diabetes and cardiovascular disease.
Alcohol intake and smoking contribute to many chronic diseases, including oral cancer. For oral cancer, there is clear evidence that smoking and alcohol together multiply the risk to a much greater extent than each does individually.
Because of the associations between other systemic diseases and periodontitis, some practitioners recommend that patients have these straightforward screening measurements recorded. However, it is always the patient’s decision whether to do so, and their right to choose is always respected.
This holistic approach to patient care was championed by BSP Past President, Dr Penny Hodge, and she kindly shared with BSP the documentation that she successfully used in practice. We have modified these documents and made them available to download:












